
Abstract: The authors describe Thresholds’ approach to offering services for high-risk young adults while at the same time providing a coordinated specialty care team for young adults with First Episode Psychosis.
"MindStrong and Emerge Models: Multidisciplinary, Feasible, Effective, and Sustainable" (2019)
Vanessa V. Klodnick, Marc A. Fagan, Ariel Brenits, Sarah Gomez, Candy Malina, Eva Zeidner, & Jose Viruet
Compared to younger youth and middle-aged and older adults, older youth and young adults (16–25 year olds) are more likely to experience serious mental health challenges, including schizophrenia, bipolar, and major depressive disorders.1 These young people are at increased risk for high school dropout (or "pushout"), unemployment and under-employment, poverty, housing instability, homelessness, justice involvement, and suicide.2 They are also least likely to utilize mental health services, which tend to feel stigmatizing, incongruent, and ineffective to young people. Accessible, attractive, and effective services spanning both child and adult sectors are needed to engage this unique population. To address these challenges, Thresholds, the largest community mental health provider in Illinois, successfully developed and implemented two multidisciplinary sister teams serving young people within a Medicaid and commercial fee-for-service insurance billing environment.
Thresholds is nationally recognized for partnering with researchers to develop and test evidence-based practices (e.g., Assertive Community Treatment, Individual Placement and Support, Supported Employment, Wellness-Management & Recovery), and for its innovative programs for older youth and young adults. In 2013, Thresholds expanded its youth care continuum by introducing a multidisciplinary, community-based model blending child and adult evidence-based and evidence-informed practices for 18- to 26-year-olds with a variety of serious mental health conditions. This model, called Emerge, utilizes the Transition to Independence Process (TIP) Model3 as its foundation and is an adapted Assertive Community Treatment model (See Figure 1). Emerge is a program without walls, where almost all services are provided in the community – wherever is relevant for learning, growth, and achieving personal goals. All participants are seen at least twice a week by their primary staff member and an additional team member. Participants build their own individualized life goals and engage in individualized in-vivo learning experiences (e.g., learning how to budget while grocery shopping or how to open a checking account with a first paycheck) with team members with a variety of disciplinary backgrounds. Therapists leverage practices from Cognitive Behavior Therapy (CBT), along with creative arts and movement-based approaches. Emerge also hosts regular, tailored social and educational meet-ups and activities in the community to foster social skills, natural peer support, and belonging.
Figure 1. Emerge Model
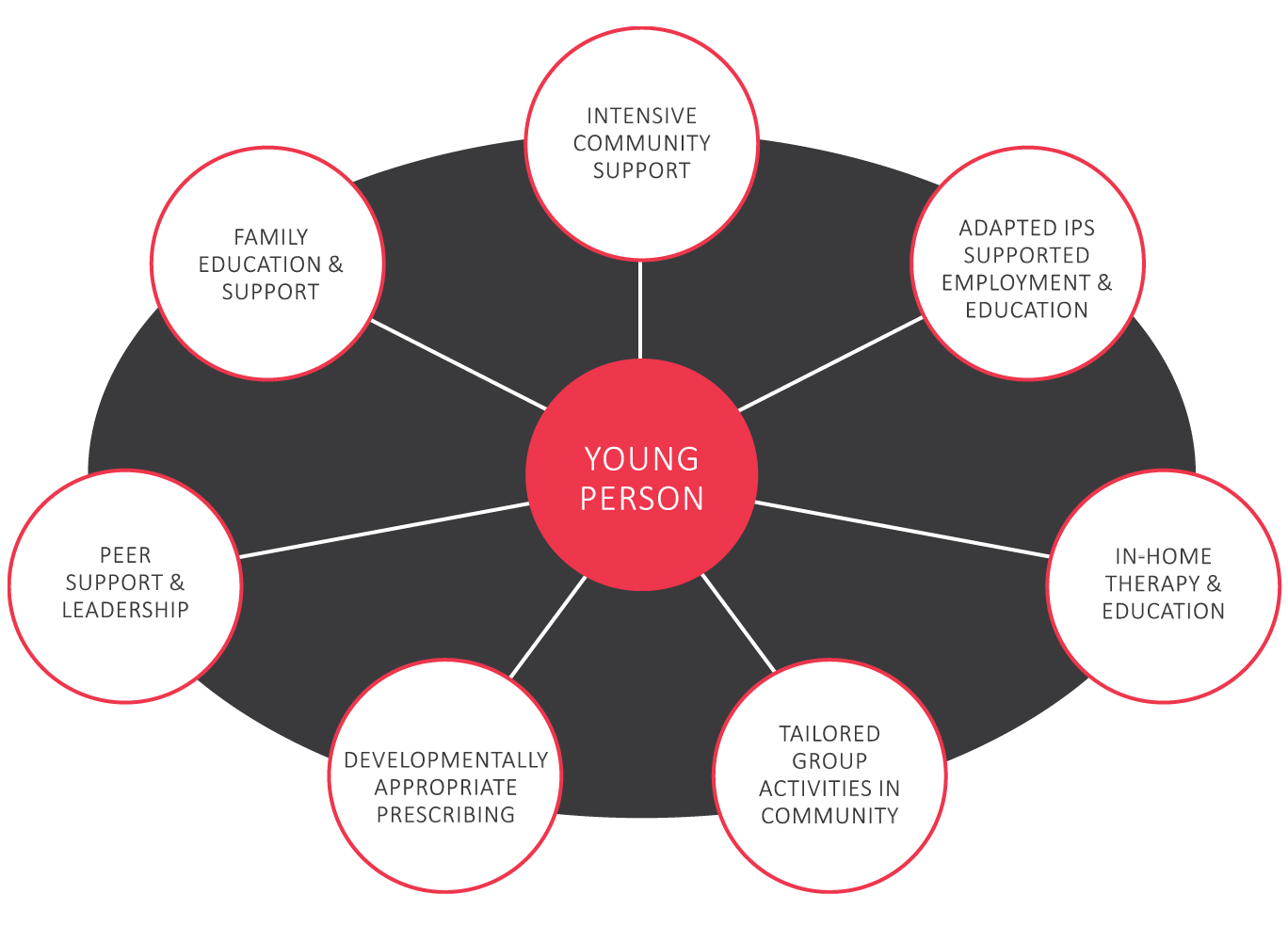
In 2016, Thresholds added a second Emerge team, and co-located a Coordinated Specialty Care team (serving those with a recent onset of psychosis) with each Emerge team. This resulted in two sets of sister teams: one set in Chicago and one in the Western suburbs. MindStrong, Thresholds' CSC team, is similar in practice and structure to Emerge and incorporates CBT for Psychosis, Individual Resiliency Training, Family Education and Multifamily Groups.4
Methods
Thresholds Youth & Young Adult Services' dedicated Evaluation, Research, and Quality Improvement (ERQI) team partners with administrators and practitioners to design feasible data collection and feedback loops. ERQI uses the Plan-Do-Study-ACT Quality Improvement Process.5 ERQI trains, coaches, and monitors staff on real-time data collection, including employment, education, and psychiatric hospitalizations, through monthly reminders, training refreshers, and quarterly meetings in which the team examines trends in these and other outcomes. For this article, we selected all participants enrolled in MindStrong and Emerge for at least one year. First, we analyzed demographic characteristics, including age, race, ethnicity, gender, and diagnoses. Second, we examined employment and education status and history, and psychiatric hospitalization history collected during intake psychosocial assessments recorded in the Thresholds electronic health record (EHR). Third, we culled all work, school, and psychiatric hospitalization life events from the EHR across service participants' first year of enrollment and summarized using counts and percentages.
Results
A total of 263 young people enrolled across the four programs since 2014. Of these, 100 remained enrolled for at least one year. Approximately 42% were African American, 38% White, 13% Latino, and 3% other. Most (63%) were male. Approximately 75% were between ages 18 and 25. DSM-V Primary diagnoses included schizophrenia spectrum disorders (42%), bipolar disorder (27%), major depressive disorder (21%), and other mood or anxiety disorders (6%). At enrollment, 40% had a high school diploma or equivalent; 20% had some college; and 10% had an associate's or bachelor's degree or training certificate. Also, at intake approximately 24% were enrolled in school (25% for Emerge; 20% for MindStrong), and 29% were employed (31% for Emerge; 20% for MindStrong). Most (86%) had been hospitalized for treatment of psychiatric disorders prior to enrollment (92% for Emerge; 73% for MindStrong).
Outcomes in First Year Enrolled
Overall, 66% were enrolled in school or employed within their first year of enrollment, with more employed (50%) compared to enrolled in school (28%). For Emerge, 64% were employed or enrolled in school within their first year of enrollment, with specifically 51% employed and 25% enrolled in school. In MindStrong, 80% were employed or enrolled in school within their first year of enrollment; specifically 47% were employed and 47% were enrolled in school.
In their first year of enrollment, overall 64% avoided psychiatric hospitalization. For Emerge, 59% avoided psychiatric hospitalization in their first year enrolled. For MindStrong, 93% avoided psychiatric hospitalization in their first year enrolled.
Discussion
The positive outcomes observed in work, school, and psychiatric hospitalizations are evidence of the positive impact of developmentally attuned multidisciplinary teams. Thresholds is an example of a real-world provider that successfully adapted, blended, and expanded practice for older youth and young adults, as well as fiscally sustained these models by knitting together funding. A number of federal initiatives, including SAMHSA's Healthy Transitions Initiatives and Mental Health Block Grant Set-Aside for recent onset of psychosis services, have paved the way for providers nationally to redesign service systems and integrate new practice models. However, many of these initiatives have not led to sustainable services because Medicaid and commercial insurance do not cover key elements of these adapted and blended models. Through robust program evaluation, service providers can demonstrate and share evidence of how adapting and blending evidence-based practice is effective for older youth and young adults. To that end, Thresholds worked with Illinois legislators to develop The Early Mental Health Act of 2018,6 which supports coverage of key service elements not previously Medicaid Reimbursable (e.g., Supported Education, Peer Support) within team- and community-based services, such as Emerge and MindStrong.
Service Model Adaptations
It is important for adult community mental health agencies to know that they can attract 16- to 25-year-olds to needed services, and achieve excellent outcomes by making adjustments for this unique population. Systematic adaptations to program structure, practices, standard operating procedures, the look and feel of where services are provided (if in office), and communication methods are important. To do this, agencies need internal champions paired with a strong understanding of transition-to-adulthood development and competency in youth engagement strategies. Early and ongoing engagement strategies are critical and translate into fiscal sustainability: more engagement, more billable hours. To engage, Emerge and MindStrong leverage key TIP Model principles:3 individualizing goal planning around what matters to young people (e.g., school, work, living situation, relationships, wellness); being flexible in where, when and how services are delivered; using young person-preferred methods of communication (e.g., texting); and using in-vivo methods relevant to life skill development rather than set curriculum. Emerge and MindStrong have embedded master's levels therapists and focus on Discovery more than Recovery. Participants engage in and benefit from services that help them to discover things about themselves. For instance, Thresholds' adapted Individual Placement and Support (IPS) Supported Employment values job endings as much as starts for gaining new insight into career and job preferences.
The rapid, national expansion of CSC for psychosis teams has created opportunity for providers to add sister teams like Emerge to meet the needs of those ineligible for CSC, but who would benefit from multidisciplinary team-based services. Emerge both complements MindStrong and serves as a referral source. Need for better understanding of how sister teams like Emerge and MindStrong blend practice and partner is immense. We aim to develop a network of providers with CSC teams and sister teams like Emerge to share practice insights and collect common outcomes to demonstrate the value of complementary and co-located teams.
References
- Substance Abuse and Mental Health Administration. (2018). Age- and gender-based populations. Retrieved from https://www.samhsa.gov/specific-populations/age-gender-based
- Munson, M. R., Narendorf, S., Zajac, K., & Cole, A. (2015). Treating common behavioral health concerns in young adulthood. In C. Juntunen (Ed.), Counseling across the lifespan, 2nd ed. (pp. 259–282). Thousand Oaks, CA: Sage.
- Clark, H. B., & Hart, K. (2009). Navigating the obstacle course: An evidence-supported community transition system. In H. B. Clark & D. K. Unruh (Eds.), Transition of youth and young adults with emotional or behavioral difficulties: An evidence-supported handbook (pp. 47–113). Baltimore, MD: Paul H. Brookes Publishing.
- National Institute of Health. (2018). What is Coordinated Specialty Care? Retrieved from https://www.nimh.nih.gov/health/topics/schizophrenia/raise/what-is-coordinated-specialty-care-csc.shtml
- Agency for Healthcare Research and Quality. (2013). Plan-Do-Study-Act (PDSA) Cycle. Retrieved from https://innovations.ahrq.gov/qualitytools/plan-do-study-act-pdsa-cycle
- Early Mental Health Act, State of Illinois Public Act 100-1016 (2018).
Suggested Citation
Klodnick, V. V., Fagan, M. A., Brenits, A., Gomez, S., Malina, C., Zeidner, E., & Viruet, J. (2019). MindStrong and Emerge Models: Multidisciplinary, Feasible, Effective, and Sustainable. Focal Point: Youth, Young Adults, and Mental Health, 33, 26–29. Portland, OR: Research and Training Center for Pathways to Positive Futures, Portland State University.